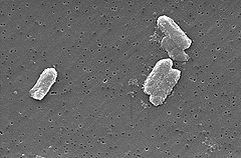
C. koseri rarely causes infection in healthy, immunocompetent patients and, thus far, has been considered an opportunistic pathogen. There were reports on infective aortic endocarditis due to C. koseri. It can also occasionally causes meningitis, sepsis, ventriculitis, and cerebritis with 80% frequent multiple brain abscesses in low-birth-weight, immunocompromised neonates.
The pathogenic mechanism is poorly understood. C. koseri may have a unique ability to penetrate, survive, and replicate into vascular endothelial cells and macrophages. Furthermore, it survives in phagolysozomal fusion and replicates within macrophages, which may contribute to the establishment of chronic abscesses
Raised serum concentrations of IgA and IgM to lipopolysaccharide (LPS) of gram-negative enterobacteria, such asPseudomonas aeruginosa, Morganella morganii, Proteus mirabilis, Pseduomonas putida, Citrobacter koseri, and Klebsiella pneumoniae have been reported in CFS patients
Psychological stress alters the gut microbiota towards decreased numbers of Bifidobacteria and Lactobacilli
People with CFS were shown to have higher concentrations of intestinal C. koseri bacteria than normal, which probably leads to higher levels of H2S. Professor Kenny De Meirleir of the Brussels Free University and his team say high levels of H2S caused by an intestinal overgrowth of Gram positive D/L lactate-producing bacteria play a major role in CFS and lead to a series of reactions in your body that leave cells devoid of oxygen and energy.
